When prospective patients start their bariatric surgery research, it can get confusing…fast. Most diet and exercise programs fail to offer long-term results on their own 5 or 10 years out, even if lots of weight is lost in the short-term. We also know that living with excess weight, especially morbid obesity, is not sustainable and is the fast track toward many serious follow-on diseases. So, how do we figure out what works and what doesn’t and most importantly the best option for our particular circumstance?
Non-surgical Versus Surgical Weight Loss
One of the first decisions we have to make revolves around the mechanism for losing weight. Non-surgical weight loss, in the form of physician supervised weight loss programs or weight loss medication, have some proven effectiveness. Many patients will lose up to 30% of their excess bodyweight and can often maintain it – but only as long as they continue the program. This is where non-surgical weight loss fails; only a small number of people are able to maintain their weight once they end the program.
Does this mean that surgical weight loss is the appropriate course of action for everyone with excess weight? No, not at all. There are well-established guidelines for patients to qualify for weight-loss surgery. Having a BMI of 35 or over with one or more diseases associated with morbid obesity or a BMI of 40 or over regardless of diseases associated with morbid obesity will typically qualify an individual. Even more importantly, the patient has to be a suitable candidate for surgery. There are anesthesia risks and other risks inherent to major abdominal surgery. The benefits of surgery must outweigh these risks.
With that being said, weight loss surgery is currently the only proven long-term solution to morbid obesity. Approximately 70 to 80% of all patients who undergo weight-loss surgery will maintain their weight loss over the course of 10 or more years. Modern surgical techniques have made bariatric surgery safer than ever with risks similar to those of a simple gallbladder removal.
Are All Bariatric Surgeries the Same? Which Is Best?
If you have decided that weight loss surgery may be right for you, the decision becomes even tougher – which bariatric procedure is best? Luckily, you will have the team here at MASJax to help you with that decision, but it is a tough one, nonetheless. Depending on a patient’s specific medical needs, one procedure may be more suited than another. For example, gastric bypass is usually most beneficial for those suffering from poorly controlled diabetes or severe acid reflux. In fact, the gastric sleeve can cause acid reflux or worsen existing reflux. However, both the bypass and sleeve are very effective for long-term weight loss as well as improving or eliminating the diseases associated with excess weight and obesity.
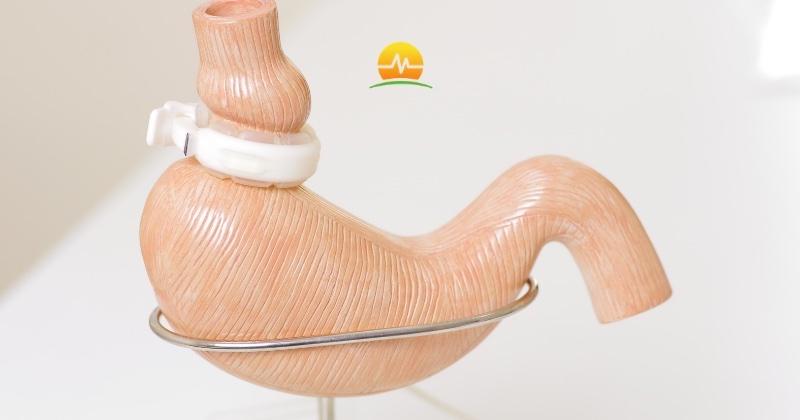
There are two popular procedures that we rarely, if ever, recommend. First is the Lap-Band or adjustable gastric band. This is a band that wraps around the upper portion of the stomach, that makes the patient feel full with less food. While it was a very popular procedure a decade ago, and is the only procedure that is fully reversible and adjustable, the long-term complications are simply too great for us to look past and recommend the band. In fact, many of the revisional bariatric procedures we perform today involve the removal of the gastric band – replacing it with a stapled bariatric procedure like the gastric bypass or gastric sleeve.
The other procedure that we do not recommend is the nonsurgical gastric balloon. During this procedure, an inflatable balloon is inserted into the stomach using endoscopy – a non-surgical technique that threads a specially made tube down the esophagus to place the balloon. The balloon is then filled with saline and takes up space in the stomach which makes the patient feel full. The balloon is left in the stomach for six months and the patient undergoes a concurrent one-year medical weight loss program supervised by their bariatric surgeon or gastroenterologist. At the end of six months, the balloon is removed. Not only is the balloon option not as effective as surgery, since it does not remain in the stomach permanently, but most insurance plans do not cover it, which means that patients pay a significant amount of money out of pocket. If they later regain weight, they have to have yet another balloon placed in their stomach, once again paid for in cash.
A Note on Going Overseas for Bariatric Surgery
There are many enticing advertisements for bariatric surgeries that are performed in other countries for a fraction of the price. While many patients choose to take this path, there are some significant potential drawbacks. Surgeons, clinical staff, and facilities overseas may not be held to the same standards as those in the United States. If complications should occur, many surgeons in the United States will not touch a procedure performed overseas. There are many unknowns about the way the surgery was performed and more often than not, patients will have to go back to their original surgeon to address non-emergency complications.
The Bottom Line
Ultimately, the decision to have bariatric surgery is a life-changing one and should be treated with the importance and seriousness that it deserves. When considering bariatric surgery, we always suggest that our patients keep an open mind and discuss their options with former patients, surgeons, and others with experience in the procedure they wish to undergo. While cost is always a consideration, it should not be the driving factor for choosing a surgeon or facility. Finding surgeons who specialize in bariatric surgery and have performed hundreds if not thousands of the procedure you wish to undergo is key to a more effective procedure with fewer complications.
We find that many of our patients benefit from attending one of our post-operative support groups, even before they decide that bariatric surgery is right for them. Attending a support group can help shed light on procedure options as well as having access to insight directly from patients who have experienced a wide range of physical and emotional ups and downs associated with bariatric surgery.