Blog Archives
Diverticulitis vs. Diverticulosis

The colon or large intestine balances hormonal secretions and keeps us healthy. Its uses are far beyond what the casual observer would consider a simple waste-collecting and bulking facilitator. However, to do its job, the colon requires a healthy balance of fiber and hydration, amongst other things. Even our habits play a role in the health of the colon. For example, straining on the toilet, sitting on the toilet for too long, and plenty of other bad habits can cause problematic changes.
When the colon is healthy, it looks like a smooth tube. Of course, there are undulations, which you’ve probably seen when looking at your results after a colonoscopy. However, small pits or cavities, known as diverticula, can form along the colon. This leads to a diagnosis of diverticulosis. Some of the most common causes of the formation of diverticula are: Continue reading
Are Green Powder Drinks Good for Bariatric Patients

In today’s world of “disruptive” foods, drinks, and supplements, there’s no shortage of options or marketing hype. One type of supplement that has made the rounds of the podcast steer. Some green powders claim to offer a barrage of benefits, from digestive health to vitamin and mineral optimization. With the podcasters and other online influencers backing some of these products, we wanted to see if they make sense for somebody in their post-bariatric surgery life. Now, it’s essential to understand that we can only offer general guidance on suitability. Every person is different. So, speak to your doctor and bariatric surgeon before changing any supplementation routine.
Why You’re Probably Consuming More Calories Than You Think and Need

One of the most complex parts of the post-bariatric surgery lifestyle is controlling and tracking how many calories you consume. However, this is also one of the most critical parts of successful, long-term weight loss. When we talk about the calories in, calories out paradigm, you might think it’s relatively easy to track through one of the many useful calorie-counting apps. However, our patients often underestimate their calories while taking far more than they need. Let’s discuss this further and see why it happens.
Why Do My Back and Joints Hurt After Bariatric Surgery?
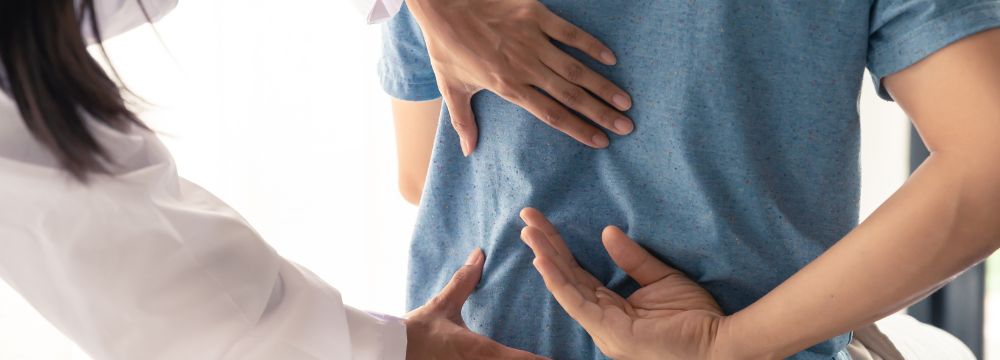
You’ve likely been told that many of the aches and pains associated with obesity are because of the excess weight and strain placed on your joints due to the added weight. Therefore, it is reasonable to believe that, as you lose weight, those joints and the pain should get significantly better. Obesity launches a two-pronged assault on the body, particularly the joints. On the one hand, the excess weight places additional strain on the joints, making it more difficult for patients to move freely and, over time, wearing away the thin cartilage layer separating bony structures. This is known as osteoarthritis. However, adipose or fat tissue also contributes to chemical releases that attack the joints and break them down further. If obesity is so bad for the joints, why then will many patients experience aches and pains after bariatric surgery?
What Is Fatty Liver Disease, and Why Does It Matter?
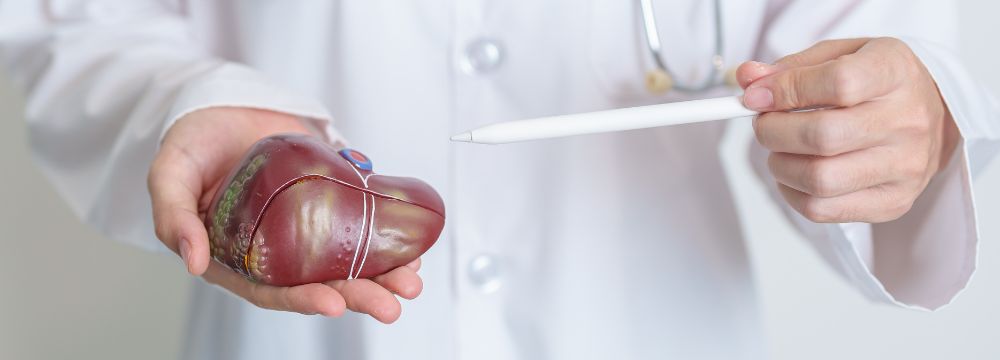
When we talk about liver disease, and in particular cirrhosis of the liver, our mind often takes us directly to alcohol. After all, we’ve been told repeatedly of the dangers of excessive alcohol consumption. There is a significant concern, both physical and psychological, associated with drinking too much. Yet, we can’t forget the fact that most fatty liver disease is not due to alcohol at all but excess weight and obesity.
Why Excess Weight Wreaks Such Havoc on the Joints

Excess weight and obesity have been definitively linked to osteoarthritis, the early degeneration of the joints. As the prevalence of obesity and morbid has increased in the United States and worldwide over the past few decades, we have seen an increasing number of patients who visit us with serious and sometimes debilitating knee, hip, and back pain. We have seen more of these patients, typically younger than in years past.
Top 10 Hurdles After Bariatric Surgery

We’re often asked about the biggest hurdles you will face after bariatric surgery. Yes, we aren’t joking when we say the hard part begins AFTER surgery. However, it is by no means impossible, and thousands of our patients who remain successful in their life changes are a testament to that. Dr. Abbas reviews the TOP 10 milestones and obstacles you will face during your weight loss journey. Get ready for them and embrace them! After all, what comes on the other side is a very sweet victory.
The Checkered History of Weight Loss Medication in the United States
Weight loss has been a perennial concern for many Americans, leading to a constant search for effective solutions. Over the years, various weight loss medications have been introduced, promising quick and effortless results. However, the history of weight loss medication in the United States is checkered, marred by controversies, safety concerns, and disappointing outcomes.
Does a Low-Carb Help Burn More Fat & Drop Weight?

As you have undoubtedly seen over the years of dieting and weight loss efforts, there is a tremendous amount of conflicting information on the Internet and elsewhere discussing how best to lose weight. We have hundreds of diets, many using gimmicks to sell a “new” narrative. However, some make more sense than others and have withstood the test of time. One classification of diets that remains popular with questionable results is the low carbohydrate kind. Low-carb has spawned hundreds of diets, some of which virtually eliminate carbs.
Let’s dive into carbohydrates and understand why the low-carb diet has been so popular.
Can You Lose Weight Without Exercising?

Diet and exercise. DIET AND EXERCISE. It’s something drilled into you from a very young age, and it’s the mantra you will hear repeatedly after bariatric surgery. Of course, while we understand that bariatric surgery is a fantastic tool, ultimately, it is up to us to maximize our results and improve our lives by eating well, moving, and stressing our muscles. The combination of proper diet and exercise is a lifestyle change. This lifestyle change is more than just a fleeting whim, it is the new normal for our patients going forward, and it is what gets them to maintain the fantastic results they may have achieved in the months and years so far after bariatric surgery.
But is diet and exercise like love and marriage? Can you have one without the other? Today we will discuss whether you can lose significant weight through diet alone, without exercising.
