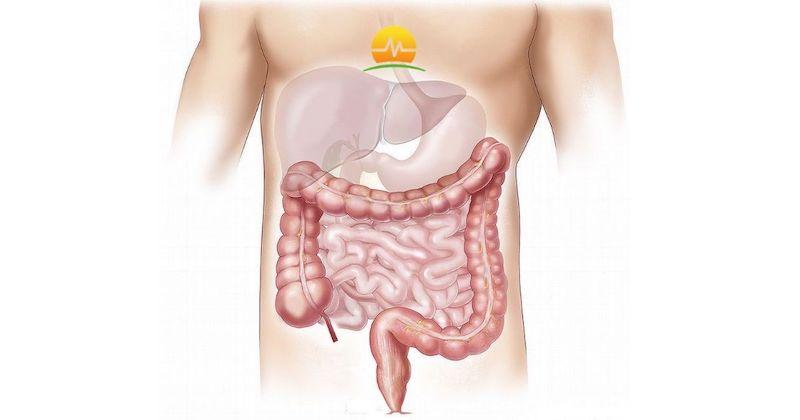
The colon or large intestine balances hormonal secretions and keeps us healthy. Its uses are far beyond what the casual observer would consider a simple waste-collecting and bulking facilitator. However, to do its job, the colon requires a healthy balance of fiber and hydration, amongst other things. Even our habits play a role in the health of the colon. For example, straining on the toilet, sitting on the toilet for too long, and plenty of other bad habits can cause problematic changes.
When the colon is healthy, it looks like a smooth tube. Of course, there are undulations, which you’ve probably seen when looking at your results after a colonoscopy. However, small pits or cavities, known as diverticula, can form along the colon. This leads to a diagnosis of diverticulosis. Some of the most common causes of the formation of diverticula are:
- Smoking
- Not eating enough fiber
- Age
- Genetics
- Excess Weight or Obesity
- Use of NSAID medication
Diverticulosis is not inherently dangerous in that these cavities do not necessarily cause problems and do not require treatment. However, when fecal matter gets trapped within these holes, it can become inflamed and infected and cause a painful infection known as diverticulitis, which can have serious ramifications.
All About Diverticulitis
As mentioned above, diverticulitis represents the inflammation of the tiny pits in the large intestine or colon, known as diverticula. Diverticulitis can be mild or severe, and the treatment plan is built on a case-by-case basis.
Symptoms of diverticulitis
The most common symptom of diverticulitis is pain in the lower left quadrant of the abdomen. This pain can be sharp or dull but almost invariably lasts for several days (and is not gas bloat or food poisoning). In some cases, especially in those of Asian descent, the pain may be more prominent on the right side of the abdomen. Many patients will experience nausea, vomiting, constipation or diarrhea. Because of the inflammation, most patients will experience abdominal pain in areas other than the lower left quadrant, and we’ll likely have a fever.
Will Diverticulitis Go Away on Its Own?
Mild cases of diverticulitis may be treated with home rest and antibiotics, but the infection may not go away without medical intervention. Further, about 1/4 of people with diverticulitis develop follow-on concerns, including abscess, bowel blockage, fistula, or peritonitis. Each of these requires urgent care, but peritonitis, caused by the rupture of inflamed diverticula, is an emergency that requires immediate care at the ER.
Treatment for Diverticulitis
As mentioned above, treating mild diverticulitis is relatively straightforward and includes antibiotics, though not all cases will require them. Patients will also be placed on a liquid diet for some time. Rest is paramount.
Occasionally, patients experience chronic cases of diverticulitis with recurring infections. At this point, surgery in the form of a bowel resection may be necessary. A bowl resection involves removing the diseased portion of the colon and connecting the two healthy ends back together. After surgery and recovery, patients will have regular bowel movements and often feel like they did before surgery.
For particularly severe inflammation, patients may need a bowel resection with a colostomy. This involves resecting the diseased portion of the bowel and connecting the upper portion to the abdominal wall where a bag collects waste. Advances in surgical technique and technology mean that, in most cases, a colostomy is reversible, and patients can have a second surgery to reconnect the bowel at some point in the future.
Prevention of Diverticulitis
Ultimately, we want our patients to prevent the progression of diverticulitis, and they can do so by following healthy lifestyle habits, including eating well (plenty of fiber), exercising regularly, staying hydrated, and avoiding smoking.
If you are experiencing any abdominal pain, you need to see a qualified physician or general surgeon. If your pain is severe and cannot be attributed to foodborne illness, you may be experiencing an emergency and need to call 911 or go to your nearest emergency room as soon as possible.
For all other non-emergent matters, we encourage you to call our office and schedule an appointment so we can adequately evaluate going to give you a diagnosis that allows for an appropriate treatment plan.