When a patient comes in for a bariatric consultation wanting the gastric sleeve, we determine if they are currently suffering from moderate to severe acid reflux. This is because new or worsened acid reflux can be a side effect of the gastric sleeve procedure. While it may seem counterintuitive, after all bariatric surgery is supposed to eliminate the most common conditions associated with obesity, how the gastric sleeve changes the gastrointestinal anatomy is somewhat different from other bariatric procedures.
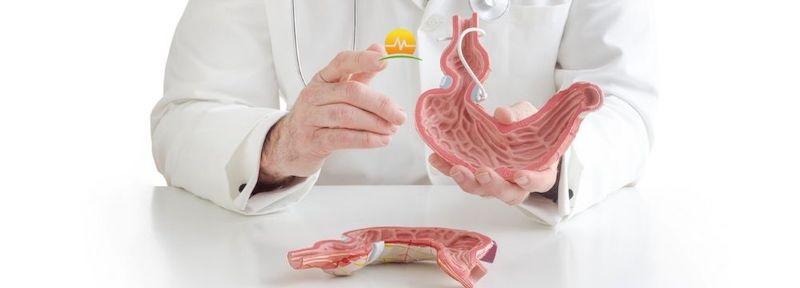
Stomach Anatomy
Think of the stomach pouch as a large pressurized tube, much like an airplane in flight. In the normal stomach, the pressure within the tube is relatively stable and gastric juices are held in place by the lower esophageal sphincter (between the esophagus and the stomach on the high end) and the pyloric valve (between the stomach and small intestine on the lower end). A functional stomach system does not allow gastric juices to go up into the esophagus and similarly does not allow the stomach contents into the small intestine prematurely.
The main cause of GERD after a gastric sleeve is simple anatomy. We are keeping the two valves at the top and bottom of the stomach intact, however we are reducing the size of the stomach by about 80%. This increases the pressure in the stomach significantly and therefore causes a greater likelihood of reflux.
The Hiatal Hernia Connection
Many obese patients also suffer from a hiatal hernia which significantly increases the risk of gastroesophageal reflux. During the sleeve procedure, we screen for a hiatal hernia and correct it if present and necessary to do so. This reduces the likelihood of post sleeve GERD significantly. For others, even this is not enough to stop reflux from occurring.
Does That Mean the Gastric Sleeve Is Not a Good Procedure?
All told, somewhere between 10 and 15% of gastric sleeve patients develop acid reflux after their gastric sleeve, when a hiatal hernia, if present, is also repaired. This is relatively low when compared to gastric sleeve patients who do not have a hiatal hernia repaired – for this group, the likelihood of developing GERD after a sleeve procedure approaches 30-40%.
The gastric sleeve, however, is so effective and straightforward that we continue to believe in it as an excellent option for most qualified patients.
With that being said, if patients are currently suffering from severe GERD we often recommend a gastric bypass procedure which, does not increase the risk of GERD.
What Happens If I Experience GERD After a Gastric Sleeve?
Patients who experience GERD after their gastric sleeve will run the gamut from mild to severe symptoms. Mild symptoms can usually be controlled with lifestyle changes including better diet and exercise. Losing weight over the course of the first couple years after surgery will also reduce the severity of GERD symptoms. However, if symptoms persist, patients today have more options than they did in the past. This is in the form of a novel, implantable device known as the LINX reflux management system. Gastric sleeve patients cannot undergo the gold standard in reflux treatment – the fundoplication – because the fundus of the stomach is removed during the gastric sleeve procedure. Oftentimes, the only option was to convert the sleeve to a bypass or duodenal switch.
However, The LINX procedure addresses this using a tiny bracelet-like implant that fits around the lower esophageal sphincter, adding pressure and reducing the likelihood of gastric juices refluxing up into the esophagus. It is a simple 20-minute procedure (not including pre-op and recovery) that can offer significant, long-term benefits.
In the end, deciding whether the gastric sleeve is the most appropriate bariatric procedure relies on this and many other questions that you will discuss with your surgeon during consultation. We encourage you to make a list of the questions and your surgeon will be able to discuss the likelihood of this and other considerations after your sleeve. We look forward to seeing you in our office for a consultation.