Inguinal Hernia Repair Surgery
 Let’s start by explaining the term ‘hernia’- which simply means an opening through which part of an organ is displaced and protrudes through the wall of the cavity containing it. Simply think of a hernia as an opening which is large enough to allow other organs, usually fat, small and large intestines to protrude through it!
Let’s start by explaining the term ‘hernia’- which simply means an opening through which part of an organ is displaced and protrudes through the wall of the cavity containing it. Simply think of a hernia as an opening which is large enough to allow other organs, usually fat, small and large intestines to protrude through it!
We then add the location where this occurs. For example, we say an ‘umbilical hernia’ that means the site of the hernia is at the umbilicus, an ‘inguinal hernia’ occurs at the groin and it can be on the left, right or both side (known as bilateral inguinal hernia). If you’ve had surgery in the past, then you may have an ‘incisional hernia’- because the surgeon made an incision in the abdomen and the tissue sutured together have come apart.
What is an Inguinal Hernia?
Inguinal hernias accounts for 75% of all the hernias seen by physicians. In the general population, males have a 25% chance of developing an inguinal hernia in their lifetime. They are not unique to males only as women can also acquire this defect, but the prevalence is much lower, the lifetime risk of developing an inguinal hernia for a female is around 3-5%.
Men are more prone to developing inguinal hernias due to the tract that the testis leave behind them as they descend from the abdomen into the scrotum, to keep them slightly cooler than the body’s core temperature and maintain healthy sperm.
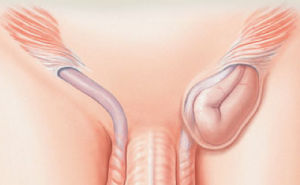
There are two openings in the abdominal wall, an opening on the inside known as the ‘internal ring’ and outer opening which allows for protrusion to the outside. The outer opening is known as the ‘external inguinal ring’ and the connection between the two rings is a short canal called the ‘inguinal canal’.
These rings are usually very small and don’t allow any of the intra-abdominal organs to come through, but if they get larger and the muscle of the lower abdominal wall weakens then fat, small and/or large intestine may protrude through the canal and a bulge will then be seen in the groin area if you strain, cough, sneeze or perform physical activity requiring effort.
How Are Inguinal Hernias Diagnosed?
Most patients have inguinal hernias diagnosed by their primary care physician on a general wellness exam or they feel a lump and seek medical attention to evaluate it. Occasionally, the hernia is discovered incidentally while performing imaging studies for unrelated symptoms. For example, you may have symptoms suspicious for gastritis and a CT scan of the abdomen and pelvis is performed. The radiologist may notice that you have an inguinal hernia of the imaging study.
Pain at the groin, whether associated with a lump or not, is also a common presenting symptom. Your surgeon or primary care physician will then perform a physical exam and if they can’t find any abnormalities but, they are still very suspicious for a hernia they may order imaging studies such as an ultrasound, MRI, or CT scan of the abdomen and pelvis.
What Causes Inguinal Hernias?
Because there are two potential weaknesses of the inguinal canal leading to two types of inguinal hernias;
Indirect inguinal hernia
This is most likely secondary to weakness or a small congenital opening. As we discussed above, in males the testes descend from the abdomen into the scrotum leaving behind an opening if this tract doesn’t close as it should.
In 2 to 3% of males it’s apparent at birth and it must be repaired. However, it may be too small to be apparent at birth, over the years the muscles may weaken due to repetitive physical activity allowing the opening to widen enough to allow fat/bowel to protrude through it. The bowel will go through the internal ring, across the inguinal canal and out the external ring. Sometimes, these hernias can be very large and extend into the scrotum.
Direct inguinal hernia
A direct inguinal hernia is secondary to weakness in the muscles of the lower abdominal wall, the intra abdominal content whether fat/small or large intestine directly pushes through the abdominal muscles and the superficial inguinal ring.
Direct inguinal hernia predominantly occurs in males, females rarely present with a direct inguinal hernia.
Do Inguinal Hernias Go Away on Their Own?
Inguinal hernias, in fact all hernias, are anatomical defects. That means the body’s normal anatomy was disrupted, leading to a hernia. As described above, in the case of inguinal hernias, it’s a weakness in the connective tissues and the muscles of the abdominal wall which.
The only way we can ‘make hernias go away’ is by fixing the defect surgically. One exception to that is a small umbilical hernia in children, where we can wait for a couple of years and see if the abdominal wall closes as they grow. In adults, that doesn’t happen as we have reached our maximal growth potential. Alternatively, the opposite occurs in older people, as we use our bodies to perform our daily activities it will lead to weakening of our muscles and connective tissues.
So, the answer to whether a hernia will go away? Unfortunately, ‘NO’.
Who is more likely/is at risk of developing an inguinal hernia?
Males are 10-15 times more likely than females to develop inguinal hernias. Males have 25% chance of developing an inguinal hernia in their lifetime compared to 2% for females. Inguinal hernias may occur at any age.
Here are other characteristics which increase the likelihood of developing an inguinal hernia:
- Those with family members who have groin hernias (genetic predisposition)
- So-called ‘‘impaired collagen metabolism’’ (collagen is a protein in many body tissues like muscle for example Ehlers-Danlos Syndrome, Marfan Syndrome, mixed Connective Tissue Disease (MCTD), etc.)
- Those with a previous hernia (this is known as recurrent inguinal hernia)
- The elderly
- Those who’ve undergone removal of the prostate gland or abdominal surgery requiring lower abdominal incision
- The obese
- Those who are extremely thin (so-called ‘‘low body mass index’’).
What Are the Signs And Symptoms of an Inguinal Hernia?
A bulge or swelling in the groin region is often the one of the first signs of a groin hernia. Pain, dragging scrotal sensation or vague discomfort may or may not accompany the bulge. The bulge, and pain if present, may worsen with straining, sneezing, coughing, lifting, exercising or standing for prolonged periods.
Occasionally, if the hernia is small, pain without bulging or swelling may indicate that a groin hernia is present. Frequently, hernias are found by your PCP on routine physical examination.
What are the complications of inguinal hernias?
Hernia ‘‘incarceration’’
If the fat/intestine caught in the hernia sac starts to swell, then it may become trapped in an abnormal location. The hernia contents then cannot return to their proper position in the body.
Hernia ‘‘strangulation’’
Strangulation is the term used after the hernia is ‘incarcerated’ for a period of time and its blood supply is compromised. If the ‘incarceration’ continues for a prolonged period, the involved bowel doesn’t have proper blood supply. This means that whatever is in the hernia bulge may begin to die.
Even though the risk of an inguinal hernia becoming incarcerated is less than 3% per year and only 5% of men with groin hernias require emergent repair. It is very important to be aware of some symptoms and signs associated with these complications, as they may become life threatening.
Worrisome Signs
- Hernia with suddenly increasing pain
- Redness of the hernia bulge and pain on touching it
- Inability to push it back (reducing the hernia)
- Vomiting or the inability to move one’s bowels can also mean that a hernia is strangulated.
Seek immediate medical attention if you have a groin hernia and develop any of the ‘‘strangulation’’ signs and symptoms listed above. You may need EMERGENCY SURGERY.
What are the Complications of Inguinal Hernia Surgery?
Groin hernia surgeries are one of the most common procedures performed in the United States. There are several factors which determine the risks and potential complications associated with an inguinal hernia repair. Some factors are related to the hernia and the patient whereas others are related to the technical parts of the procedure and the material used such as the mesh etc..
Here are a few potential complications of inguinal hernia repair, please look at them and make sure your surgeon discusses the chances of each of them occurring in your specific case:
General complications associated with any surgical intervention such as
- bleeding,
- infections,
- blood clot formation,
- pneumonia and others
Thankfully, these are all rare.
Some complications specific to inguinal hernia repair are:
- Hematoma – is a collection of blood, it doesn’t need to be extensive to cause bluish discoloration and swelling in the area of surgery, patient on blood thinner such as (Coumadin, Eliquis, Xarelto, etc. are at increased risk- hence the reason your surgeon stops these medications several days prior to your surgery and doesn’t resume them for a few days afterwards). The blood travels between tissue planes and may cause bluish discoloration of the scrotum, base of the penis, at the incision sites, or into the labia (vaginal lips) in females. This usually resolves over several days. It is usually self-limiting, and you shouldn’t be too concerned. If the swelling and bruising continues to increase, then you’ll need to get in touch with your surgeon immediately as this may be a sign of significant ongoing bleeding
- Seroma – this is clear fluid collection only, our bodies don’t like empty spaces and it fills it with sterile fluid and slowly resorbs it as the space collapses. In very rare cases the seroma needs to be drained or it may get infected. Get in touch with your surgeon if the seroma gets larger or the skin becomes red.
- Urinary retention – because inguinal hernia repair is very close to the bladder and the nerves which allows the bladder to contract, the bladder may not be able to completely empty after surgery. In this case you may feel fullness in the lower part of the abdomen, above your pubic bone and an inability to urinate. A foley catheter may need to be placed temporarily until the bladder regains its function.
- Pain – of varying degrees will occur after all surgeries. The pain is usually mild to moderate after inguinal hernia repair. We only prescribe Tylenol 500 mg and Ibuprofen 600-800 mg to be taken in combination after hernia repair surgery. In fact, we rarely prescribe narcotics to patients after an inguinal hernia repair, in fact very few patients ask for it!
- Severe chronic pain – (which is very rare – thankfully) can be debilitating and should prompt a visit to your surgeon who will advise other treatment options.
Do I need a mesh…and what about all the TV advertisements warning me about mesh complications?
Inguinal hernia surgery must be ‘tailored’ to each individual, the surgeon must be very familiar with a wide variety of techniques and select the best technique for each patient. Your surgeon will discuss the benefits and downsides of each technique and why he thinks it’s the most appropriate repair for you.
There are two general categories of hernia repair:
Open inguinal hernia repair
Your surgeon will make an incision in the groin over the hernia site and suture the defect closed. They may choose to use a mesh to re-enforce the repair or choose not to use it. There are also several meshes and mesh systems. We know from research that inguinal hernia repair without mesh reinforcement has a much higher chance of recurrence both in the short and long-term.
Laparoscopic or Robot-assisted Hernia Repair
Minimally invasive techniques have been developed to make smaller incisions, decrease pain and expedite recovery. There are several approaches to this type of repair as well. But, generally a mesh will be used in the vast majority of these cases.
Well, what about the TV ads?
Mesh is proven to be safe and is well tolerated by the human body. Ok, let’s address the elephant in the room. We too see the advertisements and as surgeons always encourage patients to ask this question. In fact, WE instigate this question if you don’t ask about it.
Ok, just like all complicated surgical issues, the answer isn’t straight forward – it depends. There are several factors to consider here; which approach is going to be used open versus minimally invasive, is this a recurrence hernia or a non-recurrent, if surgery was performed on the groin was there an infection or other complications, if a mesh is going to be used what kind of mesh is to be used and where (in which anatomical plane it’s going to be placed). Another very important factor is the patient- do you have any significant medical history i.e. do you have diabetes and how well is it controlled, bleeding disorder, heart disease, etc.
As is evident, there are many influencing factors in this equation, and you must discuss them with your surgeon. We may decide mesh repair is a good choice for one patient and may be high risk for another patient, depending on their risks and medical comorbidities.
Do I Need to Spend the Night in the Hospital?
Repair of your groin hernia may well be done as same-day surgery, which means you will not spend the night in the hospital. So, you’ll go home the day of your surgery once you are fully awake, recovered from anesthesia, able to move on your own, able to drink and feel ready to go home. Depending on your particular circumstances, groin hernia surgery can be done painlessly with local (area of the hernia only), regional (in a larger region of the body) or general (whole body) anesthesia.
Your surgeon and anesthesiologist will discuss the best anesthesia and analgesia (pain relief regimen) for you.
Related Hernia Resources
- Incisional (Surgical) Hernia
- Femoral (Thigh) Hernias
- Umbilical (Bellybutton) Hernias
- Ventral Hernias
- Hernia Surgery
- Hernia Overview
